|
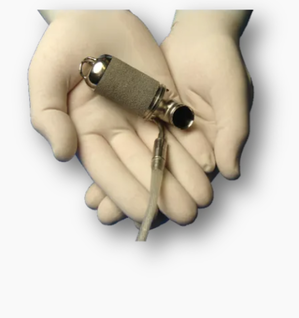
Written by: Angela Yeung ‘24 Edited by: Owen Wogmon ‘23, Surya Khatri ‘24 On May 26th, 2004, David Pierce was wheeled into surgery after a tumultuous, decade-long struggle. A retired machinist who served as a volunteer firefighter, dog rescuer, and ambulance driver, David suffered a heart attack at age 41, and was later diagnosed with congestive heart failure. Thanks to the ingenious medical device known as the left ventricular assist device (LVAD), David was able to transform into a completely “new man”— from being too weak to walk more than fifteen feet at a time, to spending time with his loved ones and mentoring other heart failure survivors. Almost 15 years post-operation, David became the longest-living patient with an LVAD [1], eventually using his experience to mentor and support other LVAD patients. Heart failure (HF) is a widespread and severe condition that impacts around 6.2 million adults in the United States [2]. The name of the illness can be misleading—heart failure does not necessarily mean that the heart itself has stopped beating, but instead indicates that the body isn’t receiving enough blood and oxygen from the heart. There are two main lines of treatment for HF: drug therapy to control symptoms and heart transplantation (to correct the disorder itself) [3]. Though heart transplantation is typically the “gold standard” when it comes to HF treatment, there is an abundance of factors that may prevent patients from being treated successfully. The most notable of these impediments is organ availability, which is often limited. Patients have to sign up on a waiting list to receive the heart transplantation procedure, and, though the one-year survival rate for patients on the waiting list has doubled from about 34% in 1987-1990 to 68% in 2011-2017 [4], many patients still do not survive. This is where the LVAD comes in, with its tremendous power to bring patients back from the brink of death. The LVAD is surgically implanted in patients who have reached end-stage heart failure and assists cardiac circulation, partially or completely replacing the function of the failing heart. The device itself is a pump that supports the left ventricle (the heart’s major pumping chamber) and assists in the mission to transport blood to the rest of the body. The typical LVAD has three major components: the mechanical pump embedded inside the left ventricle, a percutaneous (effected through the skin) driveline and an external battery-powered controller [3]. The driveline links the pump and controller, providing the LVAD with a constant flow of energy. There are two broad categories of therapy that implement LVADs— bridge-to-transplant therapy (BTT) and destination therapy (DT) [5]. As time without a heart transplant passes by, patients’ lives become increasingly compromised. The LVAD serves as a device to “buy time,” to help the patient survive until a donor heart is available to them. Depending on the patient, the LVAD may even be able to reestablish complete heart function, eliminating the need for a heart transplant. Therefore, LVAD usage through BTT is particularly useful for patients on the waiting list. On the other hand, destination therapy is targeted towards patients who may not be compatible with heart transplantation. Only when all other options (from medication, lifestyle changes, heart procedures) are exhausted do doctors utilize the LVAD for destination therapy. The goal of DT, like that of BTT, is to strengthen the pumping power of the heart. Unlike the BTT, however, there is no end goal such as a transplant surgery in mind. Instead, destination therapy aims to maintain a satisfactory quality of life for the patient for as long as possible. The first successful LVAD implantation occurred in 1966. The patient, a 37-year-old woman, underwent the LVAD surgery ten days before her heart transplantation, and the device was able to assist her heart in preserving a regular, functioning rhythm [6]. The first-generation LVADs (ex. the HeartMate XVE pump), however, posed several risks due to their large sizes and short battery lives. To alleviate these problems, biomedical engineers developed the second generation of LVADs (such as the Heartmate II and the Jarvik 2000). The devices were much smaller in size this time around, a change that resulted in a 15% increase in survival rate [3]. The third and most recent generation of LVAD, HeartWare, is exceptionally durable, making LVAD procedures much safer for both doctors and patients alike. Of course, there are a multitude of complications that could arise from the LVAD procedure. Most common risks are infection, stroke, bleeding, failure of the right heart, injuries to the kidney, and malfunctioning of the LVAD itself [7]. It was also recently reported that patients with LVADs may have increased suicide risk; unlike physical complications that are relatively easy to detect, psychological and mental symptoms also arise from the stress that comes with LVAD surgery [8]. Current studies are focused on implanting the LVAD with minimally invasive methods. As previously mentioned, the driveline for the LVAD is percutaneously implanted, which greatly increases the likelihood of infection. The use of fully implantable devices would then eliminate the need for said driveline and reduce the risk of infection [9]. We have certainly come a long way since the implantation of the first LVAD. New technology has made it possible for LVADs to shrink, become more durable, and easier to implant. As shown in David Pierce’s story, LVAD technology has shown that it can dramatically extend the period of survival in patients with heart failure. However, patients and providers are still wary, with good reason, about the potential complications that come with LVAD surgery and implantation [10]. The development of novel implantation techniques is extremely promising when it comes to further progressing the LVAD and its impact on the medical industry. Heartmate I (left) & Heartmate II (right). Jarvik 2000 Works Cited:
[1] LVAD Patient Stories [Internet]. LVAD Patient Stories | Frankel Cardiovascular Center | Michigan Medicine. Michigan Medicine; [cited 2021Feb 28]. Available from: https://www.umcvc.org/conditions-treatments/lvad-patient-stories [2] Heart Failure [Internet]. Centers for Disease Control and Prevention. Centers for Disease Control and Prevention; 2020 [cited 2021 Feb 28]. Available from: https://www.cdc.gov/heartdisease/heart_failure.htm [3] Chair SY, Yu DS, Ng MT, Wang Q, Cheng HY, Wong EM, et al. Evolvement of left ventricular assist device: the implications on heart failure management [Internet]. Journal of geriatric cardiology : JGC. Science Press; 2016 [cited 2021 Feb 28]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4984573/#:~:text=The%20very%20first%20successful%20implantation,powered%20to%20assist%20ventricular%20function [4] Bakhtiyar SS, Godfrey EL, Ahmed S. Survival on the Heart Transplant Waiting List [Internet]. JAMA Cardiology. JAMA Network; 2020 [cited 2021 Feb 28]. Available from: https://jamanetwork.com/journals/jamacardiology/article-abstract/2769179?guestAccessKey=c6f8f4ce-70f1-4b76-8649-5a2ff183364d&utm_source=For_The_Media&utm_medium=referral&utm_campaign=ftm_links&utm_content=tfl&utm_term=081220 [5] Left Ventricular Assist Device [Internet]. Stanford Health Care (SHC) - Stanford Medical Center. 2019 [cited 2021Feb28]. Available from: https://stanfordhealthcare.org/medical-treatments/l/lvad.html [6] DeBakey ME. Left ventricular bypass pump for cardiac assistance: Clinical experience [Internet]. The American Journal of Cardiology. Excerpta Medica; 2004 [cited 2021Feb28]. Available from: https://www.sciencedirect.com/science/article/pii/0002914971900762 [7] Left Ventricular Assist Devices (LVAD) [Internet]. Cleveland Clinic. [cited 2021Feb28]. Available from:https://my.clevelandclinic.org/health/treatments/17192-left-ventricular-assist-devices-mechanical-circulatory-support-mcs [8] AHA News: People With Implanted Heart Pumps May Have Higher Suicide Risk [Internet]. U.S. News & World Report. U.S. News & World Report; [cited 2021Feb28]. Available from: https://www.usnews.com/news/health-news/articles/2020-03-10/aha-news-people-with-implanted-heart-pumps-may-have-higher-suicide-risk [9] Pya Y, Maly J, Bekbossynova M, Salov R, Schueler S, Meyns B, et al. First human use of a wireless coplanar energy transfer coupled with a continuous-flow left ventricular assist device [Internet]. The Journal of Heart and Lung Transplantation. Elsevier; 2019 [cited 2021Feb28]. Available from: https://www.sciencedirect.com/science/article/pii/S1053249819313464 [10] Jefferson HL, Kent WDT, MacQueen KT, Miller RJH, Holloway DD, Hassanabad AF. Left ventricular assist devices: A comprehensive review of major clinical trials, devices, and future directions [Internet]. Wiley Online Library. John Wiley & Sons, Ltd; 2021 [cited 2021Feb28]. Available from: https://onlinelibrary.wiley.com/doi/full/10.1111/jocs.15341
2 Comments
9/3/2021 01:49:30 am
Hi. Thank you for sharing this very informative and useful article. Btw. I wanna share my experience about Genuine Haarlem Oil for Human since when I was started to using it for my health problems. Their products are very helpful both human and animals good for immune system booster.
Reply
1/18/2022 05:35:38 am
<b><a href="https://www.onegeneric.com/product/buy-lidocaine-jelly-online-intacaine-jelly"> intacaine jelly </a> </b> is a local anesthetic used to temporarily numb certain areas of the body. It is used as an anesthetic lubricant to insert instruments in the human body for medical procedures. It is also used for the treatment of symptoms of painful inflammation of the urethra and bladder.
Reply
Leave a Reply. |