|
By Olivia Woodford-Berry, '19 In order to maintain homeostasis in the case of even small stresses, the body constantly maintains a balance between proinflammatory defense mechanisms and anti-inflammatory checks. For the millions of people who suffer from autoimmune disorders, this system has lost direction. Autoimmune diseases cover a range of conditions that involve immune cells recognizing normal cells as foreign [1]. Finding effective solutions for these problems is often an uphill battle. Many such afflictions have no cure or lack reliable, long-term treatments. Historically, treatments for common conditions involve physical therapy, potent drugs, or even surgery [2]. However, research in the emerging field of bioelectronics may suggest that such drugs are not the solution. The “cure” for inflammation may be hidden within the body’s electrical language. 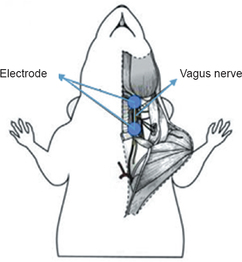 Establishing an applicable connection between the immune system and the nervous system is a project a long time in the making. Studies have demonstrated key connections in rats. Researchers found that the vagus nerve, a nerve that runs down the neck and plays a role in passing electrical signals from the brain to organs throughout the body [3], can be manipulated to regulate immune responses. For example, rats in one study were given toxins to induce an immune response and then given immunosuppressants through direct brain injections. Rats with a disconnected vagus nerves still showed an immune response everywhere but the brain. Meanwhile, rats with healthy vagus nerves showed no immune response [4]. Along the same lines, when researchers used electrical shocks to stimulate the vagus nerves of distressed rats, the rats experienced fewer symptoms of shock and produced less inflammatory signaling proteins such as tumor necrosis factor (TNF) and interleukin (IL) [5]. Scientists, in short, have stumbled upon a way to intercept and interact with electrical commands as they travel from the brain to cells throughout the body.
This study signifies a pivot point for the drug industry, especially when one considers that traditional treatments for RA cost the U.S. billions of dollars and often prove ineffective for close to fifty percent of patients [8]. While this particular case focuses on RA, this technology has the potential to revolutionize how doctors treat a wide range of autoimmune diseases. Along the same lines, bioelectronics draw attention from drug companies seeking new ways to cut costs. Since typical drugs flood the entire body, they are often extremely cost inefficient. Thus, as the cost of developing bioelectric hardware goes down, these treatments become more appealing to businesses. SetPoint, a leader in bioelectronics, has ongoing trials involving RA patients and vagus nerve stimulation [9]. They hope to produce devices that may one day be updated wirelessly, allowing patients to go years or even decades before the implant would need to be removed. While mainstream use of these technologies may seem far away, a new outlook on technology in medicine is much closer than one may think. Sources:
[1] http://www.healthline.com/health/autoimmune-disorders#Overview1 [2] http://www.arthritis.org/about-arthritis/types/rheumatoid-arthritis/treatment.php [3] http://emedicine.medscape.com/article/1875813-overview [4] http://www.nature.com/nature/journal/v405/n6785/full/405458a0.html [5] Bernik T, Friedman S, Ochani M, DiRaimo R, Susarla S, Czura C et al. Cholinergic antiinflammatory pathway inhibition of tumor necrosis factor during ischemia reperfusion. Journal of Vascular Surgery [Internet]. 2002 [cited 18 November 2016];36(6):1231-1236. Available from: https://www.researchgate.net/profile/Christopher_Czura/publication/11002713_Bernik_TR_Friedman_SG_Ochani_M_et_al_Cholinergic_antiinflammatory_pathway_inhibition_of_tumor_necrosis_factor_during_ischemia_reperfusion/links/00463529cf5010d1ff000000.pdf [6] http://www.rheumatology.org/I-Am-A/Patient-Caregiver/Diseases-Conditions/Rheumatoid-Arthritis [7] http://www.nytimes.com/2014/05/25/magazine/can-the-nervous-system-be-hacked.htmlhttp:// [8] Koopman F, Chavan S, Miljko S, Grazio S, Sokolovic S, Schuurman P et al. Vagus nerve stimulation inhibits cytokine production and attenuates disease severity in rheumatoid arthritis. Proceedings of the National Academy of Sciences [Internet]. 2016 [cited 19 November 2016];113(29):8284-8289. Available from: http://www.pnas.org/content/113/29/8284.full [9] http://www.setpointmedical.com/index.php/science/ongoing-clinical-trials
2 Comments
Susan Berry
11/29/2016 01:56:33 pm
Wow, this is great news. It's very exciting that this technology is being discovered and developed. I hope we see it being utilized soon with both RA and other autoimmune diseases. Thank you! Can't wait to read your next post.
Reply
12/3/2016 09:04:16 pm
So again I just came from CSBA in SF and one of the scientists addressing the audience noted that they had done experiments with rats where they put them into cages and exposed them to scent from sweet cherry blossoms. Then they followed that with an electric shock. The rats 'jumped'. They then took the same rats and just exposed them to the scent of sweet cherry blossom and they 'jumped', ie. although no electric shock the association was so strong that it produced the same effect. The real shocker was the offspring of the conditioned rats, who had NO exposure to any shock experiment, when exposed to the scent of sweet cherry --ALSO JUMPED! The question posed to the audience of educators, if the parents were 'traumatized' by their own educational experience, did that passed to their offspring? So perhaps not just disease but PTSD from various environmental exposures maybe could be responded to in a more effective way that just "removing the individual from the environment". Can we over come the negative environment of failure?
Reply
Leave a Reply. |

